CannMed, an event organized by Medicinal Genomics, discusses how cannabis can be used to treat pain and solve the US opioid epidemic.

The following is an article produced by a contributing author. Growers Network does not endorse nor evaluate the claims of our contributors, nor do they influence our editorial process. We thank our contributors for their time and effort so we can continue our exclusive Growers Spotlight service.
Disclaimer
This Contributors article has been reproduced with permission from Medicinal Genomics. The original article can be found here.
For far too long, opioid-based painkillers have been the go-to treatment for chronic pain of varying types. This practice has laid the foundation for the opioid crisis that currently ravages the United States.
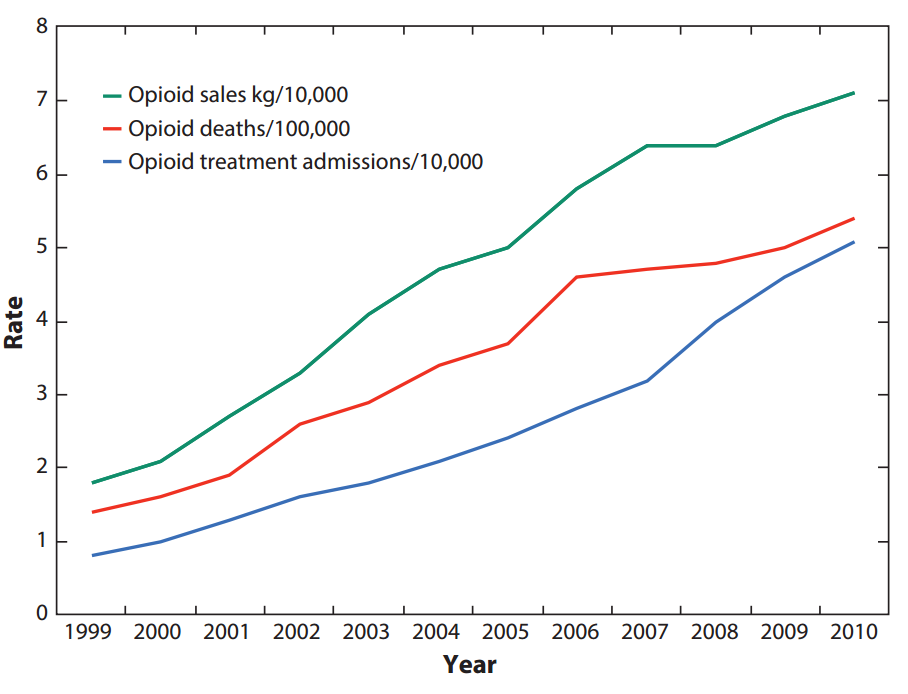
By now, you’ve probably heard the statistics, but they’re worth repeating. Of the approximately 20 million Americans struggling with a substance abuse disorder, nearly 2 million were related to the use of prescription painkillers. Drug overdose is now the leading cause of accidental death in the United States, with prescription opioid overdoses claiming the lives of 20,101 people in 2015 alone (Editor’s Note: Followed by motor vehicle accidents and unintentional falling deaths). Four out of five heroin users were initially addicted to prescription painkillers. And perhaps the most alarming figure of all; in 2012 alone, physicians wrote almost 259 million prescriptions for opioid painkillers, enough to give every adult in America a bottle of pills.
Prescription opioids are typically ingested orally where they are absorbed in our digestive tract. Opioid-based painkillers mitigate pain by binding to one (or more) of the four types of opioid receptors found in our brains. Peak effects of opioids, when taken orally, occur around 90 minutes after ingestion and their effects last varying amounts of time depending on the dose and chemical composition of the medication. According to Dustin Sulak, D.O., who presented at CannMed 2017, nearly 50 percent of opioid users were taking a short-acting opioid that put them at higher risk of abuse.
The current opioid crisis began due to a confluence of factors that appeared largely beginning in the 1990s. Those factors include physicians over-prescribing opioid-based painkillers, pharmaceutical companies promoting their products with dubious marketing practices, and patients abusing the medication they’d been prescribed. While there’s some consensus on what caused the problem, there’s less agreement on what can be done to solve it.
Editor’s Note: There’s also evidence to suggest that addictions are caused by life circumstances as well, as evidenced by Vietnam veterans returning from war.
The most commonly proposed solutions center around improving coordination in healthcare unity involvement and widespread use of alternative methods of pain management. Cannabis is one of these alternative methods, and it shows great potential in its abilities to treat chronic pain, fight the symptoms of opioid withdrawal, and even increase the efficacy of opioid treatment for patients with severe, long-lasting pain.
Editor's Note: Want to watch a video of the lecture? Check it out below.
Cannabis in Pain Management
Opioid receptors and cannabinoid receptors are both present in the region of the brain that signals pain in our bodies. These pathways have been shown to interact with each other and create similar pain-reduction effects. While opioid-based pain medications treat pain by binding to the opioid receptors in our brains, cannabis-based treatments work alongside our cannabinoid receptors to shutdown or inhibit our neural pathways that cause the sensation of pain.
Most research conducted into the use of cannabis-based derivatives in the treatment of pain have focused on acute pain. However, there is a small, growing amount of evidence to suggest that cannabinoids may be effective for the treatment of chronic pain. Due to cannabis’ classification as a Schedule I substance by the United States Food and Drug Administration, research into its potential use in the treatment of chronic pain is in its infancy; however, small-scale studies have shown considerable potential for further research. A review of 28 randomized clinical trials found “moderate-quality” evidence that cannabinoids were beneficial in treating chronic pain.
Cannabis and the Opioid Epidemic
Data presented at CannMed 2017 showed that cannabis is successful in reducing patient dependence on opioids. Dr. Sulak referenced a study conducted in Michigan with 244 medicinal cannabis patients suffering with chronic pain that found medicinal cannabis use was linked with a 64 percent reduction in opioid use and a 45 percent improvement in overall quality of life.
Once a patient becomes dependent on opioid medications, it is difficult for many to halt their opiate use due to pain reappearing and the withdrawal symptoms that accompany any addiction. Opioid withdrawal has a variety of symptoms that are commonly described as mild to severe flu-like symptoms. Commonly occurring symptoms of opiate withdrawal include:
- Diarrhea
- Nausea
- Vomiting
- Rapid heartbeat
- Excessive sweating
- Dehydration
- Seizures.
Cannabis has been shown to be effective in combating these effects and decreasing the overall severity of withdrawal symptoms. A 2013 study published in Addiction Biology found that in rats, cannabis was able to decrease the reward-facilitating effects of morphine.
Fighting the opioid epidemic will require collaboration between medical professionals, our communities, and the federal government. As pain management professionals in the United States work to ease people off of opioid-based medications, new methods of treatment will need to be brought forth to take their place. For many individuals suffering from chronic pain, cannabis may be the answer. It’s up to patients, their physicians, and thought-leaders to advocate that the federal government should reassess their stance on the medicinal use of cannabis in pain management.
The CannMed Conference is the perfect place to further the conversation about cannabis as an alternative pain management treatment. Researchers and medical professionals will present their latest findings on the topic. If you are interested in learning more about cannabis as an opioid alternative, join us at the UCLA Luskin conference center October for CannMed 2018. Check out their website if you’re interested in attending!
10 Best Gift Ideas for Cannabis Connoisseurs and Growing Aficionados (2022)
December 7, 2022Developing and Optimizing a Cannabis Cultivation System
December 14, 2021Dealing with Insomnia: How Can CBD Help?
December 10, 2020Your Guide to Sleep and CBD
December 7, 2020
Do you want to receive the next Grower's Spotlight as soon as it's available? Sign up below!
Resources:
Want to get in touch with Medicinal Genomics? They can be reached via the following methods:
- Website: https://www.medicinalgenomics.com/
- Phone: 866-574-3582
- Email: info@medicinalgenomics.com

Do you have any questions or comments?

About the Author
Ben is the Marketing Manager at Medicinal Genomics (MGC) and enjoys the challenge of trying to simplify the amazing science performed in the MGC lab into content for the layman. Ben also maintains Kannapedia.net and helps to organize and execute MGCs annual CannMed Conference. Prior to joining MGC Ben worked as an writer and editor. He earned his journalism degree from the University of New Hmapshire.
